This CE Center article is no longer eligible for receiving credits.
According to the Lucian Leape Institute’s National Patient Safety Foundation, "Workplace safety is inextricably linked to patient safety. Unless caregivers are given the protection, respect, and support they need, they are more likely to make errors, fail to follow safe practices, and not work well in teams.”1

All images courtesy of Ecore
The correct specification of flooring in health-care settings can bring a multitude of benefits to patients, nurses, doctors, and staff as well as the bottom line.
As a result of the COVID-19 pandemic, 2020 could be seen as a year of awakening. We are now collectively awakening to and more aware of the state of public health, as well as the state of our health-care system. And this will surely lead into an era of change.
Changes are likely to occur in three main areas: 1) how we view public health with attention to increasing wellness; 2) how we deliver health-care services when people get sick; 3) how we value nurses, doctors, and other health-care providers and invest in their well-being. For architects and designers who specify products for health-care settings, the years and decades ahead will be informed by what we have lived through.
Public Health and Wellness
When the pandemic hit, Americans woke up not only to the shaky foundations of our health-care system, but also to the general lack of health and wellness of our citizens as a whole, which put even more strain on our system. As the earliest fatalities caused by the novel coronavirus were reported, the term “comorbidity” became inextricably linked to the statistics. It quickly became clear that those with such existing challenges as obesity, diabetes, and asthma had a harder time surviving the virus than did citizens without those conditions and illnesses. The prevalence of obesity in the United States is more than 42 percent, up from 30 percent in 2000.2 According to the U.S. Centers for Disease Control and Prevention, “Obesity-related conditions include heart disease, stroke, type 2 diabetes, and certain types of cancer that are some of the leading causes of preventable, premature death.” Even before the pandemic, the medical cost for people who have obesity was $1,429 higher than those of normal weight. This totaled $147 billion in 2008. Never in recent memory has the cost of poor public health been so starkly observed.
But improving public health is not an easy task. While a doctor might suggest more exercise to a patient, how possible is that? Are there sidewalks in the area? Are there bike lanes? Is it safe to walk at night? What if the patient lives in a highly polluted area where breathing outside is not healthy, as is the situation with many low income and people of color? What if the rental housing is in ill repair and contains mold spores that contribute to respiratory problems?
And while a doctor might suggest that a patient eat more fruits and vegetables, are there markets with these foods in the neighborhood? Or does the patient live in a fresh food desert with only junk food and sodas available at the local store? Are there community gardens where one could grow some fresh food?
Yet despite the challenges, a heathy population will be a key component in future battles with viruses. It is likely that wellness efforts will rise to the forefront of population health strategy. Exercise, nutrition, and emotional and mental balance contribute to the wellness initiative.
When the tally has been done to calculate the cost of ill public health on both individuals and society, it is likely that the impetus toward creating a healthier citizenry will move to the forefront.

The pandemic of 2020 demonstrated the connections between fitness levels and the ability to survive the illness.
Delivery of Health-Care Services
While a healthier population will certainly ease strain on the health-care system, the system itself is poised to undergo massive changes too. Fundamental shifts are already happening, as witnessed by a tremendous—and some would say long overdue—surge in telemedicine, using video conferencing for patients to consult with health-care providers. In this scenario, the doctor, nurse, practitioner, or specialist can intersperse video conferencing with live visits for patients that need in-person evaluation. With video, patients are spared the time and expense of traveling to the location, and they are not in danger of contracting viruses from other patients in the waiting room. The downside is for patients who do not have or cannot navigate a computer, Internet access, or both.
Valuing and Caring for Nurses, Doctors, and Health-Care Providers
Of all the images the COVID-19 pandemic created, perhaps most striking was the sight of exhausted and overwhelmed nurses, doctors, orderlies, and others in the COVID-19 wards. TV and newspaper images showing these truly essential workers serving long hours day after day, often without sufficient personal protective equipment (PPE), captured the country’s attention. Without their dedication, many more deaths from the virus would likely have happened.
Nurses were especially stressed by the pandemic, as they not only cared for an onslaught of critically ill and contagious patients, but they were also tasked with comforting the dying when family members were barred from rooms due to the virus. These stresses on nurses as witnessed by the country were gut wrenching. As a result, many changes to the nursing profession are expected.
Some new awareness of nurses as a result of the pandemic include:
- Nurses have been working with fewer resources because of budget cuts and staffing shortages.
- There has been increased retirement due to concerns of catching COVID-19 in the workplace.
- Nurses have seen an increase in compassion fatigue.
- There has been a decrease in self-care.3
Changes likely to occur in the nursing profession are:
- There will be a growing public awareness of lack of nurse safety.
- There will be a focus on wellness and well-being for nurses, both in the hospital or clinic setting and outside of work.
- Nurses could be taking on more responsibilities once relegated only to doctors.
- There will be more opportunities for nurses to deliver some care and consultation via telemedicine, perhaps saving them from being on their feet for 12 hours at a time.4
Even as the pandemic unfolded, nurses started adapting on their own to prevent infections and deliver compassionate care.
One example is nurses moving IV drips and other machines toward the doorways of patient rooms so that the nurses did not have to always walk in and out of patient areas. This simple technique helped prevent the spread of the virus.
In another example, as it quickly became apparent that the use of PPE covering nurses faces except for the eyes made it hard for them to convey the compassionate care they want to deliver, some nurses taped smiling photos of themselves onto the front of their gowns so that a patient would feel the all-important human connection.
While no one knows for certain how the future will unfold in public health policy and the health-care industry, there is certainly heightened awareness about these issues. For the architect and designer, creating health-care settings that promote the health and well-being of both patients and caregivers, and an improved bottom line, will certainly be a priority. In the next section, we look at the challenges in a health-care setting that savvy specifications can help alleviate. We will use flooring as an example of products that can make the situation better.
According to the Lucian Leape Institute’s National Patient Safety Foundation, "Workplace safety is inextricably linked to patient safety. Unless caregivers are given the protection, respect, and support they need, they are more likely to make errors, fail to follow safe practices, and not work well in teams.”1

All images courtesy of Ecore
The correct specification of flooring in health-care settings can bring a multitude of benefits to patients, nurses, doctors, and staff as well as the bottom line.
As a result of the COVID-19 pandemic, 2020 could be seen as a year of awakening. We are now collectively awakening to and more aware of the state of public health, as well as the state of our health-care system. And this will surely lead into an era of change.
Changes are likely to occur in three main areas: 1) how we view public health with attention to increasing wellness; 2) how we deliver health-care services when people get sick; 3) how we value nurses, doctors, and other health-care providers and invest in their well-being. For architects and designers who specify products for health-care settings, the years and decades ahead will be informed by what we have lived through.
Public Health and Wellness
When the pandemic hit, Americans woke up not only to the shaky foundations of our health-care system, but also to the general lack of health and wellness of our citizens as a whole, which put even more strain on our system. As the earliest fatalities caused by the novel coronavirus were reported, the term “comorbidity” became inextricably linked to the statistics. It quickly became clear that those with such existing challenges as obesity, diabetes, and asthma had a harder time surviving the virus than did citizens without those conditions and illnesses. The prevalence of obesity in the United States is more than 42 percent, up from 30 percent in 2000.2 According to the U.S. Centers for Disease Control and Prevention, “Obesity-related conditions include heart disease, stroke, type 2 diabetes, and certain types of cancer that are some of the leading causes of preventable, premature death.” Even before the pandemic, the medical cost for people who have obesity was $1,429 higher than those of normal weight. This totaled $147 billion in 2008. Never in recent memory has the cost of poor public health been so starkly observed.
But improving public health is not an easy task. While a doctor might suggest more exercise to a patient, how possible is that? Are there sidewalks in the area? Are there bike lanes? Is it safe to walk at night? What if the patient lives in a highly polluted area where breathing outside is not healthy, as is the situation with many low income and people of color? What if the rental housing is in ill repair and contains mold spores that contribute to respiratory problems?
And while a doctor might suggest that a patient eat more fruits and vegetables, are there markets with these foods in the neighborhood? Or does the patient live in a fresh food desert with only junk food and sodas available at the local store? Are there community gardens where one could grow some fresh food?
Yet despite the challenges, a heathy population will be a key component in future battles with viruses. It is likely that wellness efforts will rise to the forefront of population health strategy. Exercise, nutrition, and emotional and mental balance contribute to the wellness initiative.
When the tally has been done to calculate the cost of ill public health on both individuals and society, it is likely that the impetus toward creating a healthier citizenry will move to the forefront.

The pandemic of 2020 demonstrated the connections between fitness levels and the ability to survive the illness.
Delivery of Health-Care Services
While a healthier population will certainly ease strain on the health-care system, the system itself is poised to undergo massive changes too. Fundamental shifts are already happening, as witnessed by a tremendous—and some would say long overdue—surge in telemedicine, using video conferencing for patients to consult with health-care providers. In this scenario, the doctor, nurse, practitioner, or specialist can intersperse video conferencing with live visits for patients that need in-person evaluation. With video, patients are spared the time and expense of traveling to the location, and they are not in danger of contracting viruses from other patients in the waiting room. The downside is for patients who do not have or cannot navigate a computer, Internet access, or both.
Valuing and Caring for Nurses, Doctors, and Health-Care Providers
Of all the images the COVID-19 pandemic created, perhaps most striking was the sight of exhausted and overwhelmed nurses, doctors, orderlies, and others in the COVID-19 wards. TV and newspaper images showing these truly essential workers serving long hours day after day, often without sufficient personal protective equipment (PPE), captured the country’s attention. Without their dedication, many more deaths from the virus would likely have happened.
Nurses were especially stressed by the pandemic, as they not only cared for an onslaught of critically ill and contagious patients, but they were also tasked with comforting the dying when family members were barred from rooms due to the virus. These stresses on nurses as witnessed by the country were gut wrenching. As a result, many changes to the nursing profession are expected.
Some new awareness of nurses as a result of the pandemic include:
- Nurses have been working with fewer resources because of budget cuts and staffing shortages.
- There has been increased retirement due to concerns of catching COVID-19 in the workplace.
- Nurses have seen an increase in compassion fatigue.
- There has been a decrease in self-care.3
Changes likely to occur in the nursing profession are:
- There will be a growing public awareness of lack of nurse safety.
- There will be a focus on wellness and well-being for nurses, both in the hospital or clinic setting and outside of work.
- Nurses could be taking on more responsibilities once relegated only to doctors.
- There will be more opportunities for nurses to deliver some care and consultation via telemedicine, perhaps saving them from being on their feet for 12 hours at a time.4
Even as the pandemic unfolded, nurses started adapting on their own to prevent infections and deliver compassionate care.
One example is nurses moving IV drips and other machines toward the doorways of patient rooms so that the nurses did not have to always walk in and out of patient areas. This simple technique helped prevent the spread of the virus.
In another example, as it quickly became apparent that the use of PPE covering nurses faces except for the eyes made it hard for them to convey the compassionate care they want to deliver, some nurses taped smiling photos of themselves onto the front of their gowns so that a patient would feel the all-important human connection.
While no one knows for certain how the future will unfold in public health policy and the health-care industry, there is certainly heightened awareness about these issues. For the architect and designer, creating health-care settings that promote the health and well-being of both patients and caregivers, and an improved bottom line, will certainly be a priority. In the next section, we look at the challenges in a health-care setting that savvy specifications can help alleviate. We will use flooring as an example of products that can make the situation better.
Providing Solutions in Health-Care Settings
The patient experience and outcomes must come first in a health-care setting. This is particularly relevant as Medicare and Medicaid reimbursements are tied to patient satisfaction as determined by the Hospital Consumer Assessment of Health-Care Providers and Systems (HCAPHS). This patient satisfaction survey is required by the Centers for Medicare and Medicaid Services (CMS) for all hospitals in the United States. The survey is for adult inpatients, excluding psychiatric patients. The ACA reimbursement policy is based on a “pay for performance,” outcome-based perspective as opposed to the previous “fees for services" model.
The challenges in a health-care setting must be overcome to achieve a high level of patient satisfaction. If nurses are tired and stressed, if the noise levels in the hospital are too high, if the hospital is not kept hygienic, the patient suffers, as does the bottom line.
We will look at some of the most pressing challenges in health-care settings and examine how the specification of the right flooring product can diminish these problems. But first, let’s establish the scientific basis for the correct specification.

Nurses and other health-care workers spend many hours a day on their feet. The proper specification of flooring has proven positive impacts on their health and well-being.
Health-Care Design based on Data, Not Anecdote
When using design to solve problems, the seriousness of today’s health-care needs dictates that design decisions are made based on data and not anecdotes, hype, or heresy. Two of the most respected sources for data-based design are the Center for Health Design (CHD) and the recommendation from the Facilities Guidelines Institute (FGI).
According to CHD, “The Center for Health Design advances best practices and empowers health-care leaders with quality research that demonstrates the value of design to improve health outcomes, patient experience of care, and provider/staff satisfaction and performance. Through design research, education, and advocacy, we are leading the way in transforming hospitals, clinics, wellness centers, doctor’s offices, and residential care facilities for a safer, healthier tomorrow.”
The organization’s Pebble Project, Research Coalition, and Advisory Services programs connect industry leaders with resources that help them identify the impact that investing in facility design can make.
According to FGI, its mission is to “establish and promote consensus-based guidelines and publications, advised by research, to advance quality health care.”
Both of these organizations are dedicated to evidence-based design and should be consulted when specifying to solve the problems in today’s health-care settings. Among the most pressing issues is staff fatigue.

The Center for Health Design is a trusted source for data-based specifications.

The Facilities Guidelines Institute provides guidance for designers and specifiers.
Staff Fatigue and Aging Nurses
Long before COVID-19’s impact on society, overworked and overstressed nurses were already a problem looking for a solution. Nurses are on their feet for many hours per shift, with 12-hour shifts being typical. While sore feet might be the obvious outcome, many more ailments are associated with long periods of standing and walking. According to an article in a nursing publication titled “Moving violations: negative impacts of standing and walking in nurses’ health”:
“Long periods of walking and standing are associated with plantar fasciitis, tendonitis, cumulative muscle fatigue, and varicose veins. Chronic venous disease, including primary/idiopathic abnormalities of the venous system and secondary sequelae after deep venous thrombosis, have also been associated with women who work in standing positions. In general, long periods of walking and standing without adequate rest periods is bad for your health.”5
These conditions lead to missed work and workers compensation claims many times greater than in other professions, as seen in the graph below.6
Also, the workforce in hospitals is getting older. While the valuable experience and wisdom of older workers is much needed, the risks of injury and illness are greater.
The case study on the next page illustrates both the problem of nurse fatigue and a solution in flooring specification.
Noise
When discussing the challenges of noise in a health-care setting and solutions to this problem, it makes sense to consider this quote from a report on perhaps the most influential nurse of all time:
“Florence Nightingale proposed that nursing’s major role in patient care is to produce a state of mind and body conducive to healing. She stressed nursing’s responsibility for managing the patient’s environment, assuring that the patient received adequate comfort, hygiene, nutrition, and rest.”7
Noise has long been recognized as an environmental stressor that causes physiological, psychological, and behavioral changes in healthy subjects. Environmental noise and its potential effects on healing and recovery are of special concern to nurses in hospital settings, where increased noise levels and effect of noise on patient sleep and cognitive function have been well documented.
Perhaps one of the most significant examples left behind by the founder of modern nursing, Florence Nightingale, was her commitment to patient care. She understood the importance of producing a state of mind and body conducive to healing. When it comes to designing the built environment in a way that promotes healing, the old adage “out of sight, out of mind” rings true, as acoustics are too often neglected. Yet, according to the 2015 HCAHPS scores, noise remains at the top of the list of patient complaints.8
The World Health Organization (WHO) guidelines call for continuous background noise in hospital patient rooms to remain at or below 35 dB(A) during the day and 30 dB(A) at night, with nighttime peaks no higher than 40 dB(A).9 A 2005 study examining U.S. hospital noise levels over the previous 45 years found that no facility complied with these guidelines. In fact, hospital background noise levels have been increasing since the 1960s, up from 57 dB(A) in 1960 to 72 dB(A) in 2007 during the daytime, and 42 dB(A) in 1960 to 60 dB(A) during the night.10
To better improve the healing environment for patients and providers, health-care designers and specifiers are now seeking products that feature specific acoustic benefits. While “noise” is a subjective term and can be traced to a variety of sources (hallway conversations, footsteps, rolling carts, and alarms, to name a few), hospitals and health-care facilities are working to implement sound control and mitigate sound transmission, as both play a key role in creating a healing space.
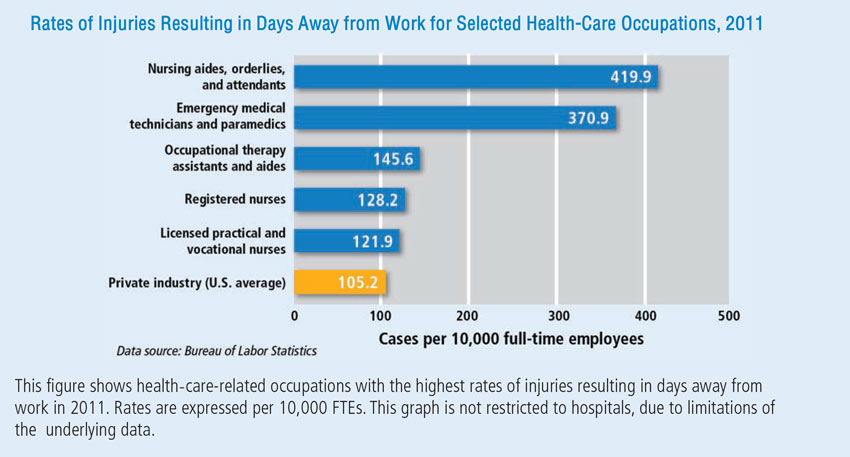
Rates of injuries resulting in days away from work are far higher for some health-care workers than for the average of the private industry labor force.
Impact of Noise on Patients and Staff
A comfortable acoustic environment is vital to supporting the safety, health, healing, and well-being of patients and providers. Patients’ physiological health can be negatively affected by poor acoustics, inhibiting the healing process and increasing their chances for readmission. High noise levels can lead to patient annoyance, sleep disruption, elevated blood pressure, and decreased healing rates.11 In terms of mental and emotional health, acoustics can impact how comfortable and secure a patient and their family members feel in the health-care setting. Loud noises that startle patients or disrupt sleep can have long-term effects, while softer sound transmission can present a lack of privacy and also cause discomfort.12
Likewise, patient care teams also feel the impact of poor acoustics. When completing tasks in a space with a high level of noise, providers may have to exert more energy to listen or be heard, which can cause fatigue and burnout. Speech intelligibility is imperative in a health-care environment, and extraneous sounds can impede providers’ abilities to understand and quickly respond to a variety of auditory signals—such as conversations, alarms, and other equipment—which affect patient care and human error.
Furthermore, HIPAA standards require that individual patient information communicated orally, written, or digitally remain private.13 When the health-care environment is finished with materials that reflect sound or is designed without acoustics in mind, discussions among patients and providers can easily carry into other areas and be overheard by an unintended listener. Poor acoustic design increases the risk of noncompliance with federal privacy regulations.
Different design strategies and technologies can be used to quiet the healing environment and minimize the transmission of sound from adjacent spaces. Products such as acoustical ceiling tiles and acoustical wall panels aim to protect patients and providers from extraneous noise by absorbing sounds from a variety of sources rather than reflecting them back into the environment. Another often overlooked component is flooring surface technology that offers noise-reducing qualities without sacrificing cleanliness or ergonomic comfort.
In the health-care environment, flooring that is hygienic and easy-to-clean is a top priority—prompting most designers to select hard surface materials for durability and cleanliness. Constant foot traffic and the movement of carts and other equipment along these surfaces, however, often create loud noises that increase sound levels throughout the facility and impact patient satisfaction. Opting for a carpet or other fibrous material that absorbs sound, on the other hand, can raise concerns of cleanliness as well as increase risks of tripping and catching when rolling carts. Recent breakthrough technology has resulted in a third option—engineered resilient flooring with a 5-millimeter vulcanized composition rubber backing—that garners the hygienic benefits of a hard surface with the acoustic and ergonomic attributes associated with carpets and other textile surfaces. These innovative materials mitigate the energy of sound, making the space seem quieter, while providing supportive cushioning underfoot to drive safety and comfort. Adding a new dimension in health-care finishes, engineered resilient flooring options are helping to create more comfortable and effective healing environments for patients and providers.

To create an environment conducive to healing, the designer should specify flooring with proven acoustical benefits.
Measuring the Impact of Flooring on Sound
To compare the effect of different flooring materials on surface-generated sound in health care, the University of Hartford Acoustics program in 2014 conducted an independent research study titled “Contribution of Floor Treatment Characteristics to Noise Levels in Health-Care Facilities.”14 Two senior acoustical engineering students chose to undertake this topic for a semester-long research project. It aimed to quantify the influence different flooring materials can have on hospital corridor noise.
While there are many noise sources within a hospital, one potentially significant source can come from the hallways and corridors, where regular traffic can include both footfall from staff and visitors, and rolling noises from medical carts and gurneys. The University of Hartford recognized that addressing these noise sources could positively affect the acoustic environment in patient rooms.
The students conducted three different tests on each surface material: an absorption test (ASTM C423), a tapping machine test, and a rolling cart test. The materials tested included carpet tiles with a vulcanized composition rubber backing, sheet vinyl, sheet vinyl with a vulcanized composition rubber backing, virgin rubber sheet, and virgin rubber sheet with a vulcanized composition rubber backing. Three of these products featured a patented technology, whereby a wear layer was fusion-bonded to a vulcanized composition rubber backing. The goal was to determine how effective this technology is in reducing noise when added to vinyl and rubber surfaces, and compare these results to standard commercial floors, such as carpet and other traditional resilient sheet products—the third option mentioned above.
The study found when a vulcanized composition rubber backing was fusion bonded with a vinyl surfacing, it was as quiet as commercial carpet when rolling a medical cart across a room or with standard footfall. An added benefit is that this surface is more conducive to meeting sanitary maintenance requirements of the healing environment. This clearly solves a multitude of problems in health-care settings.
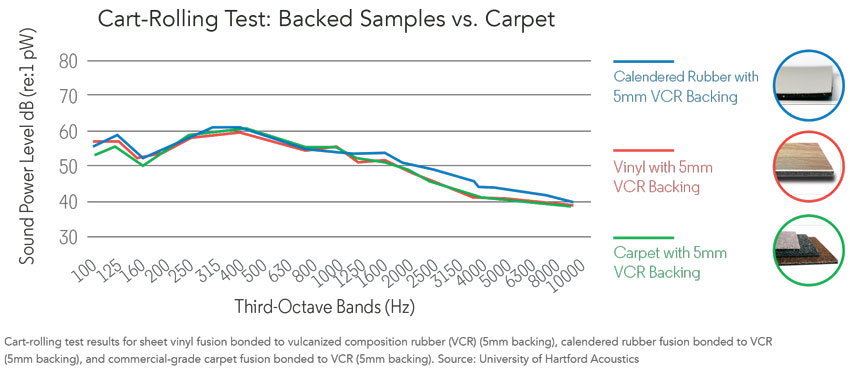
A rolling cart test at the University of Hartford Acoustics program demonstrated that when a vulcanized composition rubber backing was fusion bonded with a vinyl surfacing, it was as quiet as commercial carpet.
Ergonomics
Selecting the right surface can contribute to the comfort of the people using it, in addition to potentially reducing the risk of serious injury from a fall. When it comes to the comfort of a surface underfoot, the force reduction and energy restitution of a surface must be considered.
Ergonomic surfaces balance the absorption of force and the return of energy. Two common terms used to describe this relationship are force reduction and energy restitution.
Force reduction: This is how much energy a surface absorbs; for example, when a person walks on it. Surface of concrete would have extremely low force reduction because it absorbs very little energy, returning most of it back to the person’s feet, legs, and body.
This is tested and measured by ASTM F2569-11: Standard Test Method for Evaluating the Force Reduction Properties of Surfaces for Athletic Use.
Energy restitution: This is how much the surface returns energy. A surface of sand has very little energy restitution and high force reduction, meaning it will absorb almost all the energy and return very little back to the person’s body, making walking difficult and fatiguing.
When specifying flooring for a health-care space, it should be selected based on the force reduction and energy restitution desired for the application.
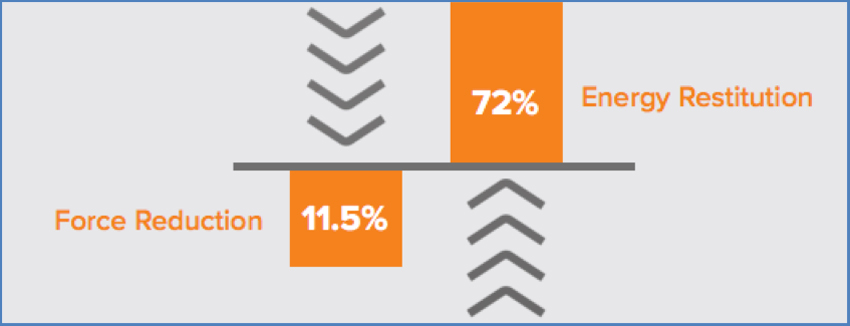
Energy restitution is how much energy a surface returns. Force reduction is how much energy a surface absorbs.
Slips and Falls
The health-care industry has been guided by long-standing requirements for coefficient of friction (COE) to prevent slips. But what has never been addressed is the actual impact that happens when a fall does occur. And falls do occur even when strict protocols are followed. Ironically, there are playground safety standards as noted in ASTM F 1292 for Height Impact Criteria. Yet no such standard exists for hospitals or senior care facilities.
Therefore, it is incumbent on the designer or specifier to pay attention to the flooring being considered and how it affects impacts. A lessened impact could make the difference between a minor and a major injury.
Hygienic surfaces
Up to this point, we are already asking a lot from our health-care setting flooring: comfort, noise reduction, fall impact reduction, etc. But there is another element that is especially critical in health-care settings in these times: surfacing that helps prevent the spread of viruses, germs, and bacteria. Flooring that helps stop the spread of pathogens must perform well on three levels: 1) be a cleanable surface, 2) be compatible with cleaning products, and 3) have welded seams.
While much attention is given to surfaces such as countertops and handrails where viruses can be transmitted from person to person, viruses can also be transmitted on flooring from room to room. Research is underway regarding the migration of microbes through shoe traffic. Specifying a flooring material that can be effectively and efficiently cleaned is more important now than ever.
Plus, the flooring surface must be impervious to the robust cleaning products used in a health-care setting. This means it should not discolor or deteriorate when cleaning products are used.
Finally, the flooring should be seamless, with welded seams impervious to topical spills and liquids, especially in the flash coving. There is a critical need for sealed floors in patient rooms and corridors.
The case study on the next page shows how the proper specification of flooring contributes to the ability of a highly respected hospital to prevent the spread of pathogens.
Specifying the Right Flooring Product for the Application
The key to savvy specification of flooring for health-care settings is to identify the needs of the client and how the specification will impact staff, patients, and residents. With the basic assumption that the flooring must meet performance standards for durability, maintainability, and both static and rolling load weights, other priorities to consider include:
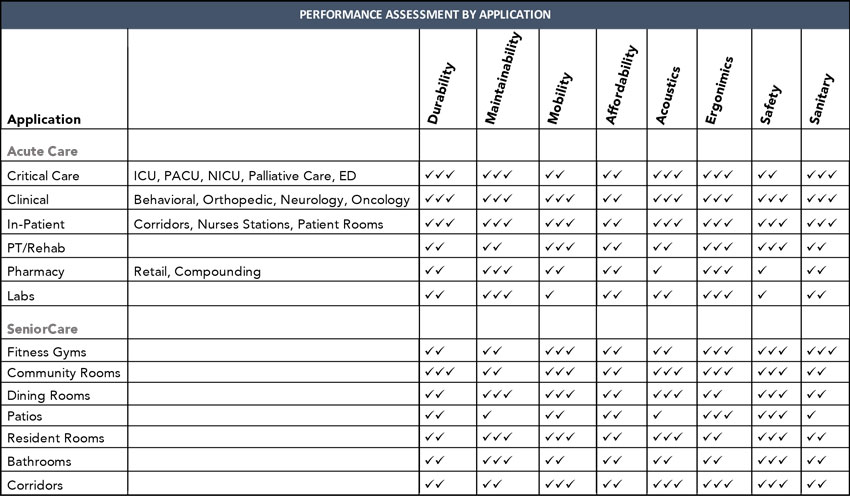
Key: √ = important, √ √ = very important, √ √ √ = critically important
Conclusion
As we have seen, there are many challenges in a health-care setting, and recent events have only heightened our awareness of these challenges. We have also seen that flooring can be part of the solution to these problems.
The bar has been raised on what flooring can do, and higher expectations must be met. New technologies in flooring can directly affect the well-being of staff, patients, and the bottom line. As a result, engineered, resilient performance surfaces featuring a VCR backing that are durable, easy to maintain, contribute to mobility, reduce noise, are hygienic, and create a safer environment must be specified in health-care applications. With this data-based knowledge, architects, designers, and specifiers now have the information they need to bring benefits to everyone who comes into contact with a health-care setting.

With data-based knowledge, architects, designers, and specifiers can choose flooring that reduces noise, creates a more hygienic environment, contributes to mobility, increases safety, and is durable and easy to maintain.
End Notes
1“Through the Eyes of the Workforce: Creating Joy, Meaning, and Safer Health Care.” Lucian Leape Institute. National Patient Safety Foundation. 2013. Web. 12 September 2020.
2“Adult Obesity Facts.” Centers for Disease Control and Prevention. Web. 12 September 2020.
3Gaines, Kathleen. “This is How COVID-19 is Changing the Future of Nursing for Students and Tenured Nurses.” Nurse.org. 26 June 2020. Web. 12 September 2020.
4Jividen, Sarah. “7 Ways COVID-19 Will Change the Future of The Nursing for The Better.” Aspen University. 21 July 2020. Web. 12 September 2020.
5Fuller, Thomas and Bain, Evelyn. “Moving violations: negative impacts of standing and walking in nurses’ health.” Massachusetts Nurse Newsletter. Massachusetts Nurses Association. 15 October 2008. Web. 12 September 2020.
6“Caring for Our Caregivers: Facts About Hospital Safety.” Occupational Safety and Health Administration. September 2013. Web. 12 September 2020.
7McCarthy, D.O.; Ouimet, M.E.; and Daun, J.M. “Shades of Florence Nightingale: Potential Impact of Noise Stress on Wound Healing.” Holistic Nursing Practice. 1991. Web. 12 September 2020.
8Kenney, L. “HCAHPS Scores, the Patient Experience, and the Affordable Care Act from the Facility Perspective.” American Society for Health Care Engineering. 22 April 2016. Web. 12 September 2020.
9Berglund, Birgitta; Lindvall, Thomas; and Schwela, Dietrich. 1999. “Guidelines for Community Noise.” Stockholm University and Karolinska Institute for the World Health Organization. 1995. Web. 12 September 2020.
10Busch-Vishniac, I.; West, J.; Barnhill, C.; Hunter, T.; Orellana, D.; and Chivukula, R. “Noise levels in Johns Hopkins Hospital.” Journal of the Acoustical Society of America. December 2005. Web. 12 September 2020.
11Hagerman, I.; Rasmanis, G.; Blomkvist, V.; Ulrich, R.; Eriksen, C. A.; and Theorell, T. “Influence of intensive coronary care acoustics on the quality of care and physiological state of patients.” International Journal of Cardiology. 15 February 2005. Web. 12 September 2020.
12Mazer, S. E. “Reduce errors by creating a quieter hospital environment.” Patient Safety & Quality Healthcare. March/April 2005. Web. 12 September 2020.
13“Summary of the HIPAA Privacy Rule.” Office for Civil Rights. U.S. Dept. of Health and Human Services. 2003. Web. 12 September 2020.
14Paul, Adam L.; Arena, David A.; King, Eoin A.; and Celmer, Robert D. “Contribution of Floor Treatment Characteristics to Noise Levels in Health Care Facilities.” The Journal of the Acoustical Society of America 2014. Web. 12 September 2020.