This CE Center article is no longer eligible for receiving credits.
Health-Impact Assessment
The public-health analogue of environmental-impact assessment, health-impact assessment (HIA), is “a combination of procedures, methods, and tools by which a policy, program, or project may be judged as to its potential effects on the health of a population, and the distribution of those effects within the population,” according to a definition developed by the World Health Organization's European Centre for Health Policy and quoted by the CDC.
HIA emerged in Europe in the 1990s and is now a rapidly growing practice in North America, with both the CDC and the Health Impact Project, a collaboration of the Robert Wood Johnson Foundation and the Pew Charitable Trusts, supporting capacity-building in its use.
HIA can be conducted as a voluntary or regulatory process to focus on issues such as obesity, physical inactivity, asthma, injuries, and social equity. It consists of six steps: screening to determine the utility of an HIA; scoping to develop a plan in consultation with stakeholders; assessment of the baseline health of, and potential impacts on, affected communities; recommendations for practical solutions; reporting of findings to decision makers and stakeholders; and monitoring and evaluation of changing health or risk factors, and the efficacy of the measures and the process.
Rapid HIAs can be completed in days or weeks; a full one may require months. In either case, it can be expected to bring to light public-health issues that might otherwise go unaddressed.
A rapid HIA began Mithun's master planning for the redevelopment of South Lincoln Homes, a 17-acre Denver neighborhood of public housing. “What we heard from the Housing Authority,” says Erin Christensen, associate principal at Mithun, “was, 'We think we're doing a good job, but we want a way to measure. We have limited resources, and we need the ability to prioritize—and to attract partners.' ”
 |
Master Plan: The Mariposa Healthy Living Toolkit helped determine the priorities for Mithun's health-integrated master plan for the revitalization of Denver's South Lincoln Homes
Image courtesy of Mithun |
The Denver Housing Authority identified health as a proxy for residents' quality of life, and commissioned the master-planning team to craft and implement a health-based development metric. The resulting Mariposa Healthy Living Toolkit, winner of a 2012 EPA National Achievement Award, customizes the HIA framework to enable design practitioners and developers to document the existing health of a community and evaluate the potential impacts of proposed redevelopment.
The Toolkit organizes health determinants into six sectors of a healthy community (housing, transportation, stewardship, social cohesion, services and amenities, and economy). For each sector, it provides objectives and rationale, indicators and strategies, references for further information, a template report card for tracking indicators, a template campaign checklist for organizing action and tracking progress, and a list of relevant organizations and potential partners.
“As designers, we have such a huge role to play in influencing health,” says Christensen. “There's all this evidence out there, so let's use it.” Mariposa's master plan replaces obsolete, inefficient housing with a mix of environmentally responsible options for a range of income levels and provides new economic opportunities in a walkable, mixed-use, transit-oriented development. When the Denver Housing Authority updated key health indicators against the rapid-HIA baseline in 2012, a 100-unit LEED Platinum apartment building was complete, subsequent building phases were in progress, and services and programs, such as community gardens, bike sharing, and health education, were under way. Even at that early stage, the monitoring found average income, crime rates, access to open space, and walking distance to healthy food outlets all beginning to show positive change.
The life expectancy of children can be predicted by their zip codes. The gist of that shocking sound bite is endorsed by experts at the Robert Wood Johnson Foundation; it forms the premise of a current exhibit at the California Museum; and it opens the report of the pilot project of the Seattle Healthy Living Assessment. Links between neighborhood design and public-health benefits are both diverse and comprehensive, as this list of examples illustrates: easier access to healthy food corresponds to lower rates of obesity and disease; mixed-use neighborhoods promote walking; proximity to parks increases physical activity; neighborhood safety corresponds to higher levels of community participation and outdoor activity; increments of income correspond to improvements in health; transportation access to employment centers affects poverty and stability; and safe, healthy, affordable housing corresponds to better health.
“The built environment affects public health at all levels of scale,” says Sharon Lerman, public-health consultant to the Seattle Healthy Living Assessment, “but the neighborhood is where it literally comes home.” The challenge for built-environment practitioners now is to act on these correspondences, to predict, evaluate, and improve the health outcomes of their work—in short, to bring public health to the design table.
For designers, a number of paradigms are emerging, some familiar—such as LEED for Neighborhood Development (LEED-ND), whose credits promote not only environmental health but public health as well—and some new, such as the growing practice of health-impact assessment (HIA). Neighborhood-scale health effects can result from regional plans, such as the Nashville Area Metropolitan Planning Organization's Regional Transportation Plan, or from a single grassroots project, such as the Watts Labor Community Action Committee's Mudtown Farms, in Los Angeles. Consultation and data have a role to play in designing for public health; so does common sense.
 |
|
Illustration by Chris Dent |
Health Checklist
The Centers for Disease Control and Prevention (CDC) Healthy Community Design Checklist is a simple, one-page listing of key components of healthy living and the neighborhood attributes that can be designed to support them.
Behind the checklist, the CDC has identified eight aspects of public health on which community design has a significant effect: physical activity; injury; access to healthy food; air and water quality; the effects of climate change; mental health; strength of social fabric; and equity of access to livelihood, education, and resources.
Of these, activity, injury, and air pollution are the most clearly understood, with solid data tracking their connections to the built environment. The remaining health factors are harder to measure. But that doesn't mean design teams should wait. “The critical thing is that [these factors] be considered, not that they be measured,” says Andrew Dannenberg, M.D., affiliate professor at the University of Washington School of Public Health, and formerly team leader of the CDC's Healthy Community Design Initiative. “I am perfectly comfortable with not measuring, and trying to do what is in the right direction.”
In fact, Dannenberg stresses that environmental designers avoid setting up a level of formality and complexity that itself becomes a barrier. “My ideal world,” he says, “is one where the design team has someone with both planning and design and public health on it. If that awareness is there, that's really sufficient.” Alternatively, he recommends that the design team “have some contact with someone who has a health background.” A 10-minute conversation could be enough to set a course in the right direction, he says: “The health issues are not that complicated.”
Green and Healthy
When the U.S. Green Building Council (USGBC), the Congress for the New Urbanism, and the Natural Resources Defense Council collaborated to develop LEED-ND, an explicit concern for the relationships between neighborhood design and health informed their work. A report prepared by a team of planning and public-health experts, “Understanding the Relationship Between Public Health and the Built Environment,” provided LEED-ND's core committee with a comprehensive appraisal of the research linking health and neighborhood design, and recommendations for integrating that knowledge into the LEED-ND rating system. The report identified links between environmental design and five categories of public health—respiratory and cardiovascular health, fatal and nonfatal injuries, physical fitness, social capital, and mental health—with a separate discussion of the disproportionate impact that neighborhood design has on vulnerable populations.
Designing for public health at the neighborhood scale often means designing for social equity. The people who benefit most from neighborhood improvements tend to be those least able to compensate for gaps in what their neighborhood provides: children, the elderly, people with limited mobility and limited income.
Public-health experts from the CDC reviewed the LEED-ND pilot version, credit by credit, for consistency with public-health research. Their work, summarized in the CDC's report “LEED-ND and Healthy Neighborhoods: An Expert Panel Review,” found that LEED-ND constitutes a “public health effort to design and build active communities that make it easier for people to live healthy lives.” It's possible, therefore, for a project to target LEED-ND certification and target health benefits by corollary.
A green-retrofitting plan for the 156-acre SALT district of the Near Westside neighborhood in Syracuse, New York, achieved Gold-level certification under the LEED-ND pilot program. The Near Westside, a mixed-use urban neighborhood of 8,400 residents, has experienced significant disinvestment for more than 50 years, leaving it the third-poorest census tract in New York state. Many of the neighborhood's historic industrial, residential, and commercial buildings are dilapidated, vacant, and/or condemned.
From an early emphasis on the environmental-sustainability aspects of the plan, the Near Westside Initiative (NWSI), a nonprofit that partnered in commissioning it, is emphasizing “more and more” the connections to public health, according to NWSI director Maarten Jacobs.
Movement on Main: Designing the Healthy Main Street, a project initiated with Syracuse University, seeks to reimagine one of the neighborhood's main streets as more walkable, safe, and engaging. In April, a design competition for the project selected a team led by Stoss Landscape Urbanism to boost movement, health, and participation in the neighborhood's emergent creative life, and to complement reinvestments along the street, such as the provision of a neighborhood health clinic and the rehabilitation of an independent grocery store.
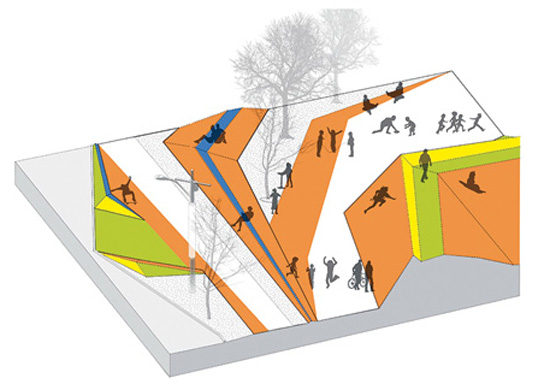 |
Movement on Main: Stoss Landscape Urbanism's winning proposal reenvisions Wyoming Street in Syracuse, New York, as a neighborhood activity center. The design configures activity mounds, seating elements, and rain gardens to encourage sitting, jumping, skipping, running, sledding, and other movement. By night, the activity continues with a play of light, colored paint, and reflective surfaces.
Images courtesy of Stoss |
Additional health-related projects completed or under development include a new playground and ball courts, improvements to pedestrian and cycling networks, and a program with the neighborhood's grocery store to enable community members to earn reward points (big points for broccoli, no points for soda) redeemable for items such as a soccer ball or a bike, and even to share their data with the health clinic if they choose.
Much of the revitalization work is still in the planning and development stages, and funding challenges are still to be met, but already there are signs of improvement, not only in the neighborhood's built fabric but in its social capital.
Jacobs attributes a good chunk of the Near Westside's rising social capital to an early and continuing emphasis on communications and art. Art-based initiatives include rezoning and retrofitting to support artists' live-work housing, as well as public art projects such as Love Letter to Syracuse, in which artist Steve Powers conducted extensive interviews in the community and painted phrases from them across bridges around the neighborhood. “I paid the light bill just to see your face,” reads one. “Now that we're here,” reads another, “nowhere else matters.”
Health-Impact Assessment
The public-health analogue of environmental-impact assessment, health-impact assessment (HIA), is “a combination of procedures, methods, and tools by which a policy, program, or project may be judged as to its potential effects on the health of a population, and the distribution of those effects within the population,” according to a definition developed by the World Health Organization's European Centre for Health Policy and quoted by the CDC.
HIA emerged in Europe in the 1990s and is now a rapidly growing practice in North America, with both the CDC and the Health Impact Project, a collaboration of the Robert Wood Johnson Foundation and the Pew Charitable Trusts, supporting capacity-building in its use.
HIA can be conducted as a voluntary or regulatory process to focus on issues such as obesity, physical inactivity, asthma, injuries, and social equity. It consists of six steps: screening to determine the utility of an HIA; scoping to develop a plan in consultation with stakeholders; assessment of the baseline health of, and potential impacts on, affected communities; recommendations for practical solutions; reporting of findings to decision makers and stakeholders; and monitoring and evaluation of changing health or risk factors, and the efficacy of the measures and the process.
Rapid HIAs can be completed in days or weeks; a full one may require months. In either case, it can be expected to bring to light public-health issues that might otherwise go unaddressed.
A rapid HIA began Mithun's master planning for the redevelopment of South Lincoln Homes, a 17-acre Denver neighborhood of public housing. “What we heard from the Housing Authority,” says Erin Christensen, associate principal at Mithun, “was, 'We think we're doing a good job, but we want a way to measure. We have limited resources, and we need the ability to prioritize—and to attract partners.' ”
 |
Master Plan: The Mariposa Healthy Living Toolkit helped determine the priorities for Mithun's health-integrated master plan for the revitalization of Denver's South Lincoln Homes
Image courtesy of Mithun |
The Denver Housing Authority identified health as a proxy for residents' quality of life, and commissioned the master-planning team to craft and implement a health-based development metric. The resulting Mariposa Healthy Living Toolkit, winner of a 2012 EPA National Achievement Award, customizes the HIA framework to enable design practitioners and developers to document the existing health of a community and evaluate the potential impacts of proposed redevelopment.
The Toolkit organizes health determinants into six sectors of a healthy community (housing, transportation, stewardship, social cohesion, services and amenities, and economy). For each sector, it provides objectives and rationale, indicators and strategies, references for further information, a template report card for tracking indicators, a template campaign checklist for organizing action and tracking progress, and a list of relevant organizations and potential partners.
“As designers, we have such a huge role to play in influencing health,” says Christensen. “There's all this evidence out there, so let's use it.” Mariposa's master plan replaces obsolete, inefficient housing with a mix of environmentally responsible options for a range of income levels and provides new economic opportunities in a walkable, mixed-use, transit-oriented development. When the Denver Housing Authority updated key health indicators against the rapid-HIA baseline in 2012, a 100-unit LEED Platinum apartment building was complete, subsequent building phases were in progress, and services and programs, such as community gardens, bike sharing, and health education, were under way. Even at that early stage, the monitoring found average income, crime rates, access to open space, and walking distance to healthy food outlets all beginning to show positive change.
Urban Scale
The obesity epidemic and rise in chronic disease are now “so great, so dire, and such an emergency,” says Anna Ricklin, manager of the American Planning Association's Planning and Community Health Research Center, “that we've got to figure out better solutions. It has to be a significant, multipronged approach [with participants] interacting with people they haven't historically worked with.”
Ricklin points to the Nashville Area MPO's 2035 Regional Transportation Plan (RTP) as an example of what she's calling for. Winner of a 2012 National Transportation Planning Excellence Award for its groundbreaking work in integrating health priorities into transportation planning, the RTP uses public-health criteria to help prioritize transportation-project funding.
Sixty of 100 points by which transportation projects are ranked for financial support depend on improvements to air quality, active transportation, injury reduction, personal health, equity of transportation facilities in underserved areas, and proximity to neighborhood services and amenities. As a result, 70 percent of adopted roadway projects in the 2035 plan include active-transportation components such as bike paths, sidewalks, and greenways—up from 2 percent of projects in the previous plan.
In addition to the scoring criteria, staff recorded how many food sources were located within a mile of each of the 500 proposed projects, and whether there were high concentrations of low-income, minority, or elderly populations in the same area; this information weighed in the funding allocations.
Furthermore, the MPO conducted training for regional and community leadership on the subjects of complete streets and school-siting policy. It conducted the area's first-ever comprehensive regional bicycle and pedestrian study of existing conditions, and modeled latent demand. It established health-related standards for transit-oriented development and championed a transportation and built-environment focus area in the Tennessee Obesity Taskforce's Eat Well, Play More program.
“The most significant thing we did?” says Leslie Meehan, the MPO's director of healthy communities. “We passed policy without having the data.” Meehan sees other departments hesitate because they can't collect health data or don't know how to interpret it—but, she says, the health implications of food deserts, no sidewalks, and dangerous intersections are common sense. “Change your policy, change your priorities, put your funding behind it, and see what happens,” she says. “Then monitor, and publish.”
The city of Seattle has a history of neighborhood-scale planning. Its Healthy Living Assessment (HLA) tool, which won a 2013 National Planning Achievement Award, builds on that history to develop another example of a significant, multipronged approach to the need for health-integrated planning.
The HLA collects data not only on a neighborhood's physical characteristics but on how people live in it, how they use it. “For planners used to thinking in terms of zoning and building heights, the HLA requires a bit of a shift,” says Sharon Lerman, health consultant to the project, “to step back and really, intentionally, put the people in, and figure out their best interest.”
With that objective, the HLA consists of three data-gathering tools and a template for synthesizing the data collected. The first tool comprises a set of detailed questions to assess the status of key health indicators: food access, mobility and physical activity, and community stability. The second tool is a neighborhood questionnaire designed to generate information not available elsewhere: how people perceive neighborhood safety, for example, and how they get to the grocery store. And the third tool is a set of questions for community discussion.
“Framing the conversation around people and how they live their lives was game-changing for us in terms of community engagement,” says Nora Liu, manager of community development at Seattle's Planning and Development Department. The reports that emerged from two pilot projects provide nuanced, humane portraits of neighborhood character and its impact on residents' lives. Moreover, residents have taken on the implementation of the resulting neighborhood plans “in a way that I have never seen,” says Liu.
Development of the HLA also helped foster the city's institutional capacity for addressing health and the built environment through interdepartmental collaboration. “We bring all the different folks to the table,” says Liu. “For some, it's the first time they've sat in a room together.”
Grass Roots Change
Links between public health and the built environment also offer a lever for community-initiated change. In South Los Angeles, the Watts neighborhood has a history of poverty and civil unrest. A median household income of around $25,000 supports—or, more accurately, doesn't support—a population with one of the county's highest percentages of children. Watts is located between the port of Los Angeles and downtown L.A., but the food trucks drive through without stopping, and residents must drive 20 to 40 minutes for fresh food. Rates of obesity, heart disease, and diabetes run high.
“What's the role of the architect here?” asks Michael Pinto, design principal at Osborn Architects. “We can look at parties thinking about similar things, but not communicating. We can put out a vision that might get people to start talking to one another.”
In collaboration with the Watts Labor Community Action Committee (WLCAC), Pinto has led students from the Southern California Institute of Architecture and Woodbury University to focus on a central 2.5-acre cultivation site in Watts. The team developed a series of speculative propositions by which Mudtown Farms could become a nucleus for nourishing the community. They envisioned a security fence growing free food, a community kitchen producing goods labeled “made in Watts,” a transit-stop market, streetlights, and bike lanes. They linked food production with job creation, education, land use, civic space, community development, urban infrastructure, safety, and health.
“Architects have the ability to zoom out and then zoom back in,” which enables them to transcend the divisions of public policy, says Pinto. “Working speculatively and putting out visions, we've been successful at getting diverse support.”
 |
Farming Fence: “Let's not just do a fence,” says Michael Pinto of Osborn Architects. For Mudtown Farms, Pinto's students at Woodbury School of Architecture proposed a food-growing, light-shining, exchange-promoting, crime-deterring, placemaking fence to improve the connectivity and walkability of a neighborhood.
Image courtesy of Juan Collantes, Melissa Reyes, Art Marquez/Woodbury University |
In April 2012, California State Parks awarded the WLCAC a $4.9 million grant to implement Mudtown Farms. “What this means to the community is self-determination,” says Janine Watkins, a WLCAC volunteer instrumental in driving the project forward. “To have local food access is more essential than a hospital for us, more essential than medicine. The health reasons for this project hit every mark—spiritual, physical, mental. It is a whole wellness concept. And it is a humble attempt to give power back to the people.”
Paradigms to Come
For its 2013–14 Mark Ginsberg Sustainability Fellow, the USGBC has appointed a physician and public-health researcher, Matthew Trowbridge, assistant professor at the University of Virginia School of Medicine, who is working to promote cross-disciplinary conversations and advance public-health priorities through design. Trowbridge's work on the Buckingham County Primary and Elementary School in Virginia contributed to that project's healthy foodscape (see story on page 66) and the CDC's Healthy Eating Design Guidelines for School Architecture.
“The structure and discipline of a design tool forces us to make our public-health knowledge practical and applicable,” says Trowbridge. “We need to keep working to translate [public-health research] into usable forms, and get it into the hands of the green-building industry, which is perfectly positioned to take it forward.” What if health priorities could become something like a LEED credit, he wonders aloud. And how would you do that?













