Eight Fundamental Performance Characteristics of Healthcare Flooring Specification
EBD PERFORMANCE CHARACTERISTIC #3: REDUCE NOISE LEVELS24
Noise is an adverse event; it is neither benign nor considered neutral.25 Flooring is a critical component within a larger system of environmental factors that can either contribute to an adverse auditory event or support reductions in ambient noise.26 In the healthcare environment, evidence suggests that increased noise levels can have a measurable impact on both the patient and staff experience.27 For patients, increased noise levels have been found to contribute to an increased length of stay and medication use as well as affect wound healing due to increased sleep disturbances.28 Research also suggests elevated noise levels can lead to emotional exhaustion of caregivers as well as increased fatigue and staff burnout.29 Furthermore, “Quietness of the Hospital Environment” has consistently been rated across the United States as one of the lowest-rated items on the HCAHPS survey, reinforcing the need to further evaluate design strategies for interior finishes, of which flooring plays a major role to focus on reducing unwanted ambient noise in the built environment.30
Part of the solution is to create a culture of quiet. To achieve that, the World Health Organization (WHO) established a limit of continuous background noise in a room of 35 decibels (dB) during the day and 30 dB at night. Hospital noise exceeding 30–35 dB levels is a factor in sleep deprivation, sensory overload, and reduced comfort levels of patients.
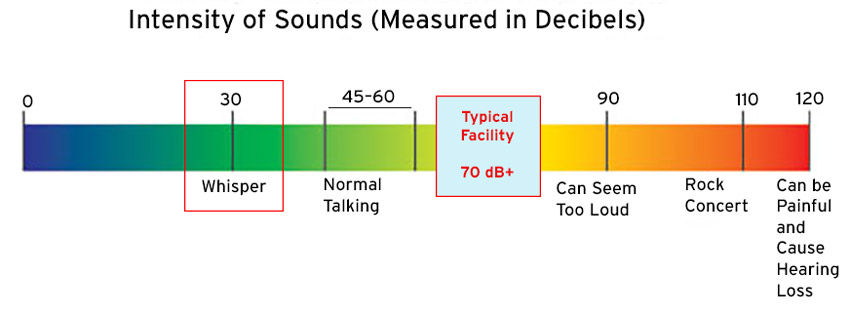
Image courtesy of Interface
The typical healthcare facility is at 70 dB, far above the guideline recommended by the WHO.
The FGI Guidelines for Design and Construction of Hospitals, 2018 Edition mentions that floors should be selected with consideration to acoustic properties to help preserve sleep and protect privacy and accuracy of communication in support of HIPAA compliance and medical error reduction. See Section 1.2-6.1.3: Design Criteria for Acoustic Surfaces and Section 1.2-6.1.6: Design Guidelines for Speech Privacy.
Flooring specification has an immense impact on ambient noise reduction in healthcare settings. The proper flooring selection actually improves the perception of quietness and can help mitigate sources of noise that can’t be avoided.
In a third-party study for in-room impact noise reduction conducted by the University of Salford, Manchester, United Kingdom, a premium rubber floor and commercial carpet tile were found to be equal at a 21 dBA sound reduction (A-weighted decibels, abbreviated dBA, are an expression of the relative loudness of sounds in air as perceived by the human ear), dampening unwanted sound more effectively than other resilient floors that ranged from 3 to 7 dBA. Findings from this study provide tangible evidence for architects, designers, stakeholders, and project teams that the type of flooring material specified can significantly contribute to reducing impact noise for building occupants.
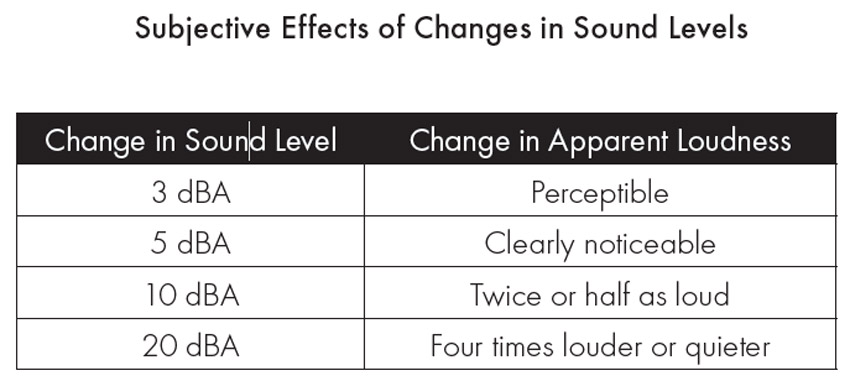
Source: Reynolds (1981) and Long (2006)
The changes in apparent loudness are perceptible at varying intensities. A change in sound levels results in subjective effects.
Dependent on space-specific needs, acoustically, carpet tile can be an alternative to other types of flooring, offering five times more sound absorption than hard surfaces like vinyl composition tile (VCT).
Look for LVT with acoustic backing that is certified for its superior noise-reduction qualities, offering best-in-class performance for reduced impact sound in outpatient and post-acute care spaces.
When acoustics is improved, noise reduction can have a positive impact on verbal communication, pain management, incidents of readmission, length of stay, caregiver retention and attention to detail, and patient experience.
EBD PERFORMANCE CHARACTERISTIC #4: REDUCE STAFF FATIGUE33
The nursing profession is the largest segment of the nation’s healthcare workforce totaling 3.6 million workers.34
“Nurses are the consummate caregivers, often sacrificing their own health and wellness while taking care of others.”
—American Nurses Association, 2017
Overall, $21 billion in cost is due to medical errors in the United States. Roughly $14 billion cost is caused by human factors at a rate of 70 percent. According to the Centers for Disease Control (CDC), medical errors rank as the third top cause of death.

Source: Shanafelt, Boone, Tan et al, 2012, 2015; SOA/Milliman/HFMA, 2016; CDC, 2015
Burnout and stress cause medical errors and cost health systems billions of dollars.
There is a direct correlation between stress, burnout, and patient safety. Nearly half of nurses exhibit substantial symptoms of work-related burnout. Turnover among RNs with less than two years of experience is at 51 percent. At an average cost of $49,000 and 86 days to fill per RN turnover, the average hospital loses $6.4 million annually in turnover costs.35
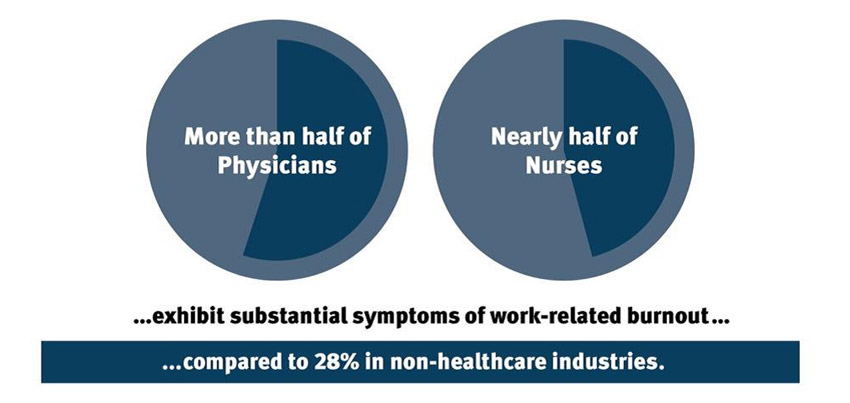
Source: Shanafelt, Boone, Tan et al, 2012, 2015; McHugh et al, 2011, 2014
The percentage of physicians and nurses who suffer from work-related burnout far surpasses those who work in non-healthcare industries.
We cannot enhance the patient experience without also considering and improving the caregiver experience. Patients instantly feel the impact of having to interact with a burned-out caregiver, and it is reflected in HCAHPS scores. Caregiver experience is linked to clinical quality and performance. Since caregiver stress and burnout are reaching unprecedented levels, this directly impacts revenue. Given that 70 percent of medical errors are due to burnout, and all of these impact clinical efficiency and operational costs, the built environment and its interior-finish selection must be facilitators, not barriers, to reducing fatigue. Floorcoverings can have an actionable impact, as noise is a major contributor to cognitive fatigue.
Why is burnout in nursing so prevalent? Nursing is a physically, cognitively, and psychologically demanding career.36 Overall, the workforce is aging. Fifty-one percent of the current workforce is over age 40, which is a 33 percent increase since 1980. Forty percent of the U.S. workforce is age 50 or over.37
And nurses walk a lot. According to one study, nurses walk between 1 and 5 miles per 10-hour shift, depending on the time of day or night.38 That much walking can lead to fatigue and burnout. Should carpet be the right solution, traditional backings provide the right amount of cushion and comfort for everyday situations, but when greater cushioning is desired, look for a cushion backing that offers superior underfoot comfort without sacrificing performance.
The day-to-day effects of standing for long periods of time can be debilitating and painful for the caregiving staff. In the healthcare setting, researchers identified hazards associated with prolonged standing in the nursing profession.39 They include “leg pain, spinal compression, chronic venous insufficiency, increased risk of heart carotid atherosclerosis, and impaired circulation, which in turn can lead to varicose veins, decreased oxygenation, increased fatigue, pain, and adverse birth outcomes.”40
The research links flooring and shoe features to the side effects associated with prolonged standing. It described the dilemma of flooring design decisions: Generally, when a person stands for long periods, softer floors provide less muscle fatigue and more comfort than hard floors, especially for the lower extremities and lower back. Floor material that is too soft, however, will affect stability and may increase muscle demands and fatigue.41 Flooring selection can have an actionable impact on reducing musculoskeletal fatigue and injury.
Floor surfaces should allow easy movement of all wheeled equipment to be used in the facility. The exertion required by staff to move equipment or beds may increase with the use of carpet; however, different types and brands of carpet may have significantly different levels of resistance to wheeled devices. Installation of a mockup to test flooring materials in relationship to wheeled equipment and devices used in a facility is recommended. In the FGI Guidelines, it states that carpet should not be automatically discounted as inappropriate due to this challenge, as it has major advantages over hard-surface flooring in terms of noise reduction and acoustics.
The study suggests that flexible flooring materials (e.g., rubber, carpeting, cork, and wood) support safer standing than inflexible flooring materials.









